
Workers’ compensation can feel a little different when the employer manages the whole process on their own. In self-insured workplaces, the employer assumes the role that an external insurer, such as iCare, typically handles. They fund the claim, manage the paperwork, and coordinate your recovery from start to finish.
Even within a self-insured model, employee rights do not change. Employees continue to receive the same entitlements under self-insured workers’ compensation in NSW, and all claims must still comply with SIRA self-insurer obligations. The only difference is how the claim management process operates behind the scenes.
Most self-insured employers choose this model because it allows faster decisions and more direct communication. It also places a bigger responsibility on them to manage injuries properly, which is why many partner with Workplace Rehabilitation Providers (WRP) like AusRehab to support safe, compliant recoveries and help workers return to meaningful duties sooner.
A self-insured workplace is an organisation that manages and funds its own workers’ compensation claims. Instead of paying premiums to an external insurer like iCare, the employer handles the entire process internally. The rights of workers do not change. Every injured worker stays covered under the NSW Workers’ Compensation Act.
Only large and financially stable employers can become self-insured. They must hold a SIRA self-insurer licence, meet strict safety standards, and report their performance each year. Some employers run their own internal claims teams. Others outsource parts of the process. The employer still stays responsible for compliance, recovery progress, and return-to-work outcomes.
This setup creates a more direct relationship between the worker, the employer, and the rehabilitation provider. It also places clear expectations on the employer to offer suitable duties, support medical treatment, and maintain a strong return-to-work program.
💡 Did you know? Only employers with proven financial strength and certified WHS systems can hold a SIRA self-insurer licence. This protects workers and ensures the employer can meet all injury management obligations.
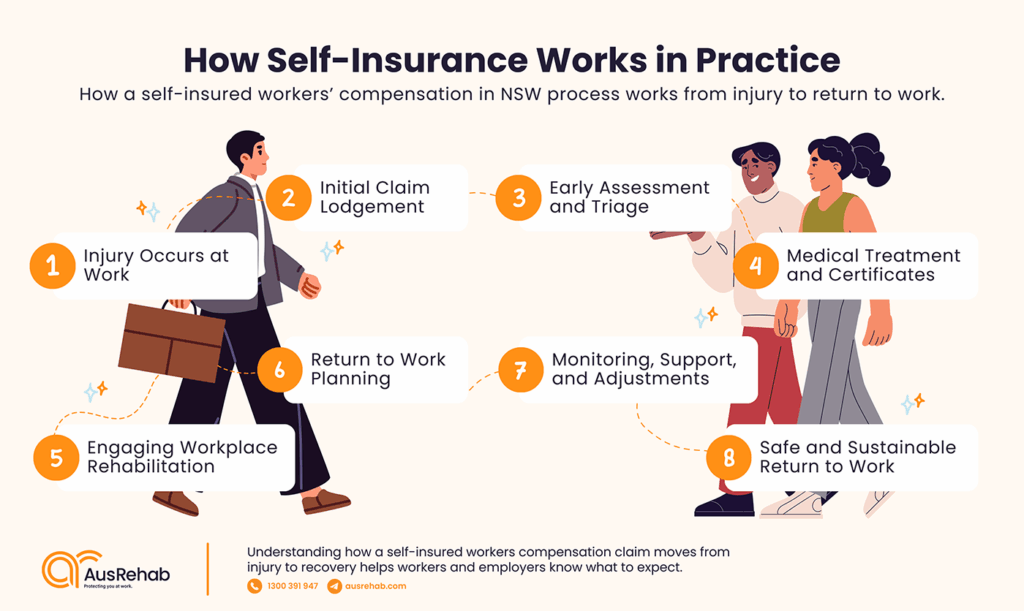
Understanding how a self-insured workers’ compensation claim moves from injury to recovery helps workers and employers know what to expect. The process is straightforward. Each step is handled inside the organisation, with support from medical providers and workplace rehabilitation where needed.
Self-insurance operates under the same legal framework as standard workers’ compensation in NSW. The main difference is who manages each part of the claim. This table of comparison shows how responsibilities shift between a self-insured employer and an iCare-managed workplace.
Process Stage | Self-Insured Employer | iCare-Managed Employer |
Claim lodgement | The internal claims team receives, reviews, and manages the claim. | External insurer (iCare) reviews the claim, makes decisions, and manages approvals. |
Medical management | The employer coordinates treatment, approves providers, and manages all medical needs directly. | The insurer allocates providers, approves treatment, and oversees medical costs. |
Rehabilitation and RTW | The self-insurer engages a WRP, like AusRehab, and internally approves, funds, and oversees the RTW plan. | The employer may request a WRP, while the insurer (iCare) approves, funds, and manages the RTW plan and rehabilitation services. |
Oversight | Compliance is monitored through SIRA audits, licence obligations, and annual reporting. | iCare conducts compliance reviews and monitors employer obligations under the scheme. |
Workers in self-insured workplaces follow the same basic claim steps as any other NSW worker. The main difference is that the process happens inside the organisation instead of through an external insurer. Workers still receive medical support, wage benefits, and rehabilitation services. The employer manages the claim, coordinates treatment, and partners with workplace rehabilitation providers to support a safe return to work.
Self-insured employers take on more control of the claims process, which means they must meet strict compliance requirements. Every organisation with a SIRA self-insurer licence must maintain systems that protect workers, support recovery, and keep claims aligned with NSW workers’ compensation laws.
A key part of the obligations of self-insured employers in NSW is maintaining strong injury management processes. This includes clear reporting pathways, timely claim decisions, coordinated medical treatment, and an active Return-to-Work Program that offers suitable duties whenever possible. These requirements help injured workers stay connected to work and recover safely.
Compliance also extends to financial and workplace safety. Self-insured employers must show stable financial capacity, maintain certified WHS systems, and submit regular audits to SIRA. These checks confirm that the employer can fund claims, manage risks, and support safe recovery.
Top Compliance Essentials:
Self-insured employers must follow the same legislation as any other NSW workplace. They must manage claims fairly, provide suitable duties through strong return-to-work programs in self-insured workplaces, and meet all SIRA reporting, audit, and financial obligations. They remain fully responsible for claim outcomes, even when they use external partners for support.
Workers in self-insured companies receive the same workers’ comp entitlements in NSW as any other employee in the scheme. Self-insurance only changes who manages the claim. It does not reduce or limit the workers’ compensation benefits employees are entitled to under self-insurance arrangements. Employees still have access to medical treatment, weekly payments, workplace rehabilitation, and fair claim decisions.
All claim decisions must comply with the NSW Workers’ Compensation Act. Even when the employer manages the claim internally, the legislative standards remain unchanged. Employees may seek clarification, request reviews, or use the SIRA dispute process if they disagree with a decision. Employee rights in self-insured workplaces remain fully protected under NSW law.
💡 Employee Rights:
Employees are entitled to:
Workers have identical rights and entitlements to those under a standard workers’ compensation policy. They can access treatment, receive income support, challenge decisions, and request workplace rehabilitation assistance. Self-insurance does not reduce or restrict any worker benefits.
Both employers and workers share the benefits of self-insurance in workers’ compensation. Since everything is handled within the organisation, decisions are made faster and support is organised without waiting for an external insurer. This helps workers receive treatment sooner and improves overall recovery outcomes.
For self-insured employers in NSW, managing claims directly creates accountability. They see the real cost of injuries, which encourages stronger early intervention and better injury management practices.
Workers also benefit because the claim is handled by people who understand the workplace, the duties available, and the adjustments that can genuinely support recovery. This leads to improved recovery outcomes in NSW and more realistic return-to-work plans.
Here’s a summary table showing the benefits of self-insurance in workers’ compensation for both employers and workers:
Benefits for Employers | Benefits for Workers |
✅ Faster claim decisions and approvals ✅ More accurate oversight of injury management costs ✅ Tailored rehabilitation solutions that reflect real job demands ✅ Stronger control of recovery plans and workplace adjustments | ✅ Quicker access to treatment and support ✅ Return-to-work plans built around actual workplace needs ✅ Clearer communication with a team that knows the environment ✅ Greater consistency during the recovery process |
Self-insurance allows employers to manage claims directly, which leads to faster decisions and earlier support. Workers receive timely treatment and more personalised return-to-work planning. Employers benefit from improved recovery outcomes and reduced long-term claim costs.
Workplace rehabilitation is essential for self-insured employers because it creates a clear structure for recovery and keeps claims moving. Early assessments and coordinated planning reduce disputes, shorten claim duration, and support safer return-to-work planning in NSW. It also helps employers meet SIRA requirements through consistent documentation and evidence-based decisions.
A strong rehab process keeps workers engaged in suitable duties and sets realistic expectations for recovery. It improves communication between employers, workers, and treating providers, which leads to smoother and more sustainable RTW outcomes. Effective early intervention workplace rehab also prevents small issues from becoming long-term claims.
These services provide objective information, guide safe duties, and support vocational rehabilitation in NSW when alternate roles are needed.
Service | Purpose | Benefit |
Objective work-capacity test | Clarifies safe duties, reduces disputes | |
Identify suitable duties | Keeps the worker connected to work | |
Alternate career planning | Shortens long-term claims | |
Prevent re-injury | Improves workplace safety |
Workplace rehabilitation supports self-insured employers by providing structured recovery pathways, objective assessments, and clear RTW planning. It ensures duties match medical advice, prevents delays, improves communication, and strengthens compliance. Early rehab involvement reduces long-term claim risks and leads to better recovery outcomes for workers and employers.
AusRehab plays a key role in helping self-insured employers manage injuries through early intervention, structured planning, and clear communication. The team delivers workplace rehabilitation services that align with SIRA standards, ensuring accurate documentation, compliant reporting, and consistent support for every claim.
We help reduce claim duration by identifying safe duties early and addressing barriers before they escalate. Regular updates keep employers informed, while workers receive timely assessments, practical guidance, and a clear plan back to meaningful duties. This approach supports sustainable return-to-work outcomes and helps employers manage claims efficiently.
AusRehab supports self-insured employers through early intervention, workplace assessments, functional and vocational assessments, and coordinated RTW planning. The team ensures duties align with medical advice and documentation meets SIRA requirements. Workers benefit from timely support, structured rehabilitation, and access to vocational services that help them return to safe and suitable work.
Strong injury management and early workplace rehabilitation are the backbone of effective self-insured workers’ compensation in NSW. When systems are clear and proactive, workers recover sooner and employers face fewer risks. Early intervention also supports smoother decisions, safer duties, and consistent SIRA compliance.
AusRehab helps self-insured employers build stable and cost-efficient programs. The team provides clear assessments, tailored support, and structured return-to-work programs that keep workers engaged and help employers maintain a reliable, compliant process.
Contact AusRehab today to strengthen your self-insured rehabilitation system and support your workers with confidence.
Self-insured employers are regulated by SIRA NSW. SIRA issues licences, audits injury management systems, and checks financial and WHS performance. Self-insurers must follow the same legislation that governs all self-insured workers’ compensation providers in NSW.
Yes. Self-insured employers often engage AusRehab to support injury management and return-to-work planning in NSW. External providers help maintain impartial assessments and consistent recovery outcomes.
Yes. Workers have the same dispute rights as any other employee under the NSW scheme. They can request a review through SIRA or proceed to the Personal Injury Commission if needed.
Workplace rehab strengthens compliance by providing accurate assessments, clear documentation, and structured return-to-work plans. This supports SIRA audit requirements and improves the quality of injury management systems
Self-insurance gives employers more control over costs and claim decisions. Internal management reduces delays and supports early intervention. This often lowers claim durations and improves overall WHS performance.
Early intervention speeds up treatment, supports accurate planning, and prevents long-term claims. It also reduces disputes and helps workers transition back to safe duties sooner.
AusRehab assists with workplace assessments, functional testing, vocational assessments, and return-to-work coordination. The team provides structured rehab plans that align with SIRA expectations. This helps employers manage complex or high-risk claims with confidence.
Rehab providers document capacity, workplace risks, and duty recommendations with clarity. This strengthens evidence for SIRA audits and demonstrates that injury management duties are completed properly.
Yes. Self-insured employers must follow the NSW Workers’ Compensation Act. Workers have the same entitlements, rights, and access to support as those in iCare-managed workplaces.
Don’t forget to share!
Subscribe to stay updated on the latest workplace news.

Resolve your work
place injury today